85% % of hip fractures in people older than 65 This traction has an external pin distal to stabilized area Pulse use a doppler if you can't palpate this fascia can't expand to increased pressure surgical fasciatomy age, type of fx, bone quality factors considered for hip fx treatment out of bed This should happen on post op day 0 Pallor sign of arterial insufficiency below level of injury Risk factors for compartment syndrome trauma, plaster cast, ortho postops, burns, infected limb Early mobilization decreases mortality rate after ortho post op This should never be placed under the knee after TKA neurovascular assessment focus areas (5Ps) neurovascular assessment assessing nerve function and blood flow to injured extremity ORIF open reduction internal fixation Buck's traction Pain Worry if this is out proportion to injury - - not relieved by meds fat particles lodge in vessel BKA below the knee amputation aspirin, SCDs, TED hose lovenox DVT prophylaxis Paralysis Late sign of prolonged nerve compression or muscle necrosis something to reduce risk or hip fracture Osteoporosis and falls Risk factors for hip fx Paresthesia decreased sensation, hypersensation - result of nerve compression 1-3 days after injury (usually femur) when trauma pt will typically develop fat embolism 85% % of hip fractures in people older than 65 This traction has an external pin distal to stabilized area Pulse use a doppler if you can't palpate this fascia can't expand to increased pressure surgical fasciatomy age, type of fx, bone quality factors considered for hip fx treatment out of bed This should happen on post op day 0 Pallor sign of arterial insufficiency below level of injury Risk factors for compartment syndrome trauma, plaster cast, ortho postops, burns, infected limb Early mobilization decreases mortality rate after ortho post op This should never be placed under the knee after TKA neurovascular assessment focus areas (5Ps) neurovascular assessment assessing nerve function and blood flow to injured extremity ORIF open reduction internal fixation Buck's traction Pain Worry if this is out proportion to injury - - not relieved by meds fat particles lodge in vessel BKA below the knee amputation aspirin, SCDs, TED hose lovenox DVT prophylaxis Paralysis Late sign of prolonged nerve compression or muscle necrosis something to reduce risk or hip fracture Osteoporosis and falls Risk factors for hip fx Paresthesia decreased sensation, hypersensation - result of nerve compression 1-3 days after injury (usually femur) when trauma pt will typically develop fat embolism
(Print)
N-% of hip fractures in people older than 65
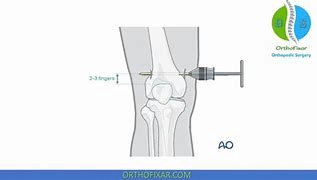
N-This traction has an external pin distal to stabilized area
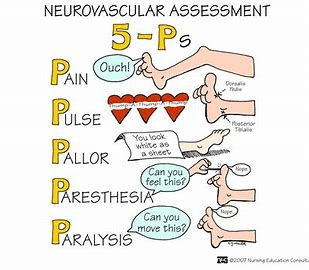
G-use a doppler if you can't palpate this
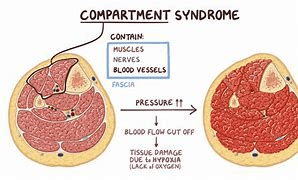
B-fascia can't expand to increased pressure
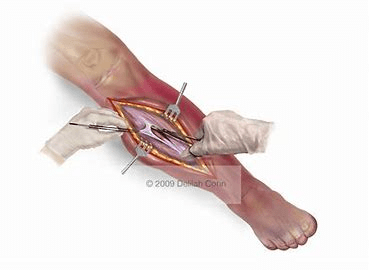
O-surgical fasciatomy
B-factors considered for hip fx treatment
O-This should happen on post op day 0
G-sign of arterial insufficiency below level of injury
B-trauma, plaster cast, ortho postops, burns, infected limb
I-decreases mortality rate after ortho post op
G-This should never be placed under the knee after TKA
I-neurovascular assessment focus areas (5Ps)
O-assessing nerve function and blood flow to injured extremity
I-open reduction internal fixation
G-Buck's traction
N-Worry if this is out proportion to injury - - not relieved by meds
B-fat particles lodge in vessel
I-below the knee amputation
O-DVT prophylaxis
N-Late sign of prolonged nerve compression or muscle necrosis
O-something to reduce risk or hip fracture
B-Risk factors for hip fx
I-decreased sensation, hypersensation - result of nerve compression
G-when trauma pt will typically develop fat embolism